
Improve the way you walk
Science has shown that the more you move, the healthier you are. The simple act of walking a few extra steps per day can make all the

Inner knee pain? Here are some of the top causes, symptoms, diagnoses, and treatments
Inner knee pain (aka medial knee pain) can show up at the oddest times and can make a normal outing feel more like an inconvenience
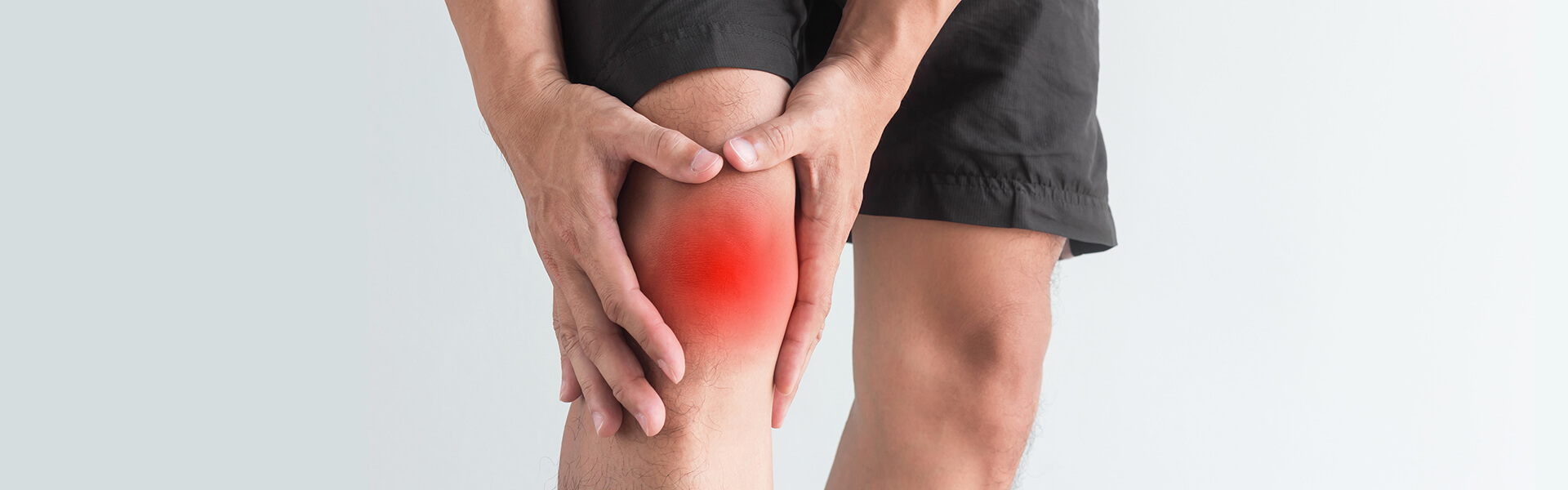
Deep Knee Pain? Here’s What You Need to Know About Causes, Symptoms, and Potential Treatment Options for Pain Inside the Knee Joint
It can be exhausting trying to figure out where our aches and pains come from. Pain inside the knee joint is no different! Whether the

How Long Does It Really Take to Lose Weight?
One of the most asked questions about weight loss is how long it will take to lose weight. Let’s face it, struggling to lose weight

2021 Report on Arthritis and the Impact of the Pandemic
Arthritis impacts the lives of more than 54 million adults and 300,000 children in the US, being deemed the nation’s number one cause of disability.

An Introduction to Gait and Gait Abnormalities
Have you ever had knee, hip, back, or leg pain? Maybe the better question is—who hasn’t? Whether you are currently suffering from chronic pain or

10 Ways to Treat Chronic Knee Pain
We’ve all experienced physical pain in some capacity or another. At the moment that we’re injured, and for some time after, the pain can be

How Your Gait Cycle Impacts Your Health
The big gait cycle question. Can changing the way you walk relieve chronic pain? Before you sit down to read this, get yourself a glass

What Walking Speed Says About Your Health — and Longevity
We often think of medicine in the context of treating people who are already sick or injured—that’s when most of us go to the doctor.
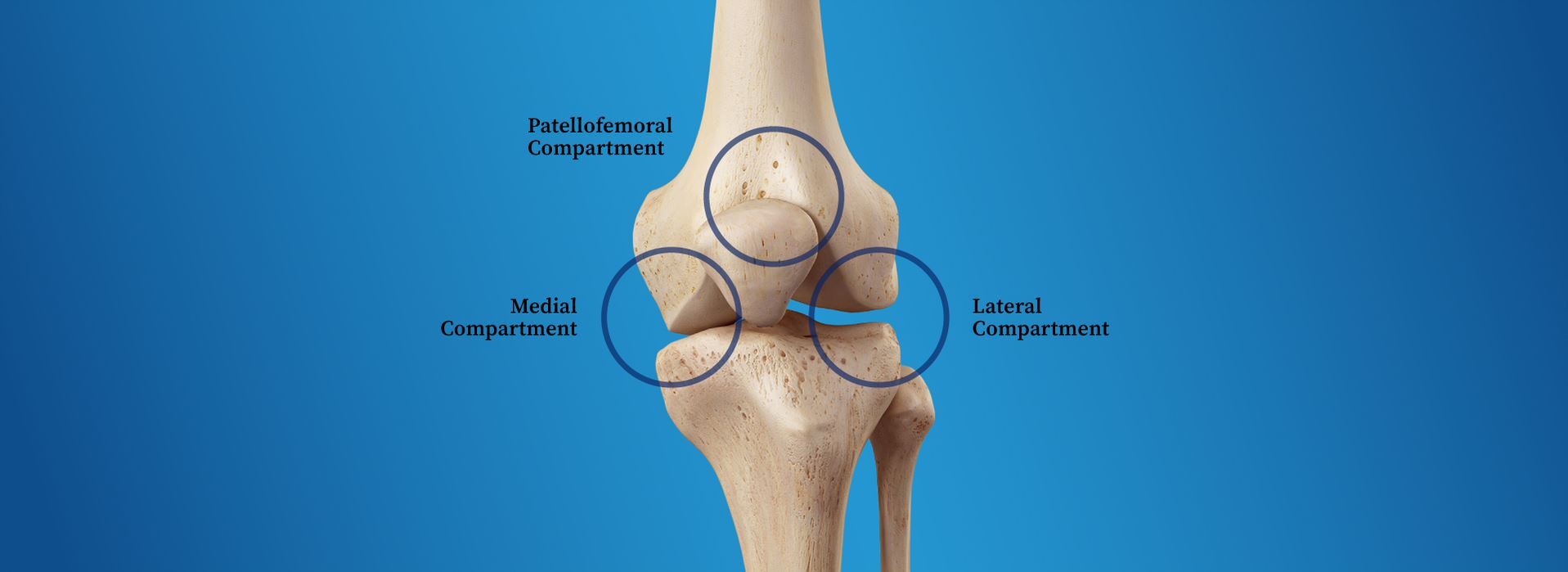
What is Tricompartmental Osteoarthritis? – Here’s What You Need To Know
Tricompartmental osteoarthritis is the most complex type of knee osteoarthritis and affects only 1.5% of knee osteoarthritis sufferers. Fortunately, there are ways to address it and manage it, including at

Is Foam Rolling Effective for Knee Pain?
If you’ve been suffering from knee pain, you might have heard of foam rolling. Foam rolling is on the rise as a popular treatment for

Double Trouble: How to Break the Knee Pain/Weight Gain Cycle
All too many people who suffer from knee pain find themselves trapped in a vicious cycle of being unable to exercise due to knee pain,

Relieve Joint Pain Through Diet
Foods to Reduce Joint Pain Living with joint pain can be difficult and tiresome. Disruptions to your daily routine and limitations resulting from pain and

10 Healthy Ways to Celebrate Grandparents Day in 2020
In case you hadn’t heard, National Grandparents Day falls on September 13 every year, and it’s the perfect time to focus on taking steps to
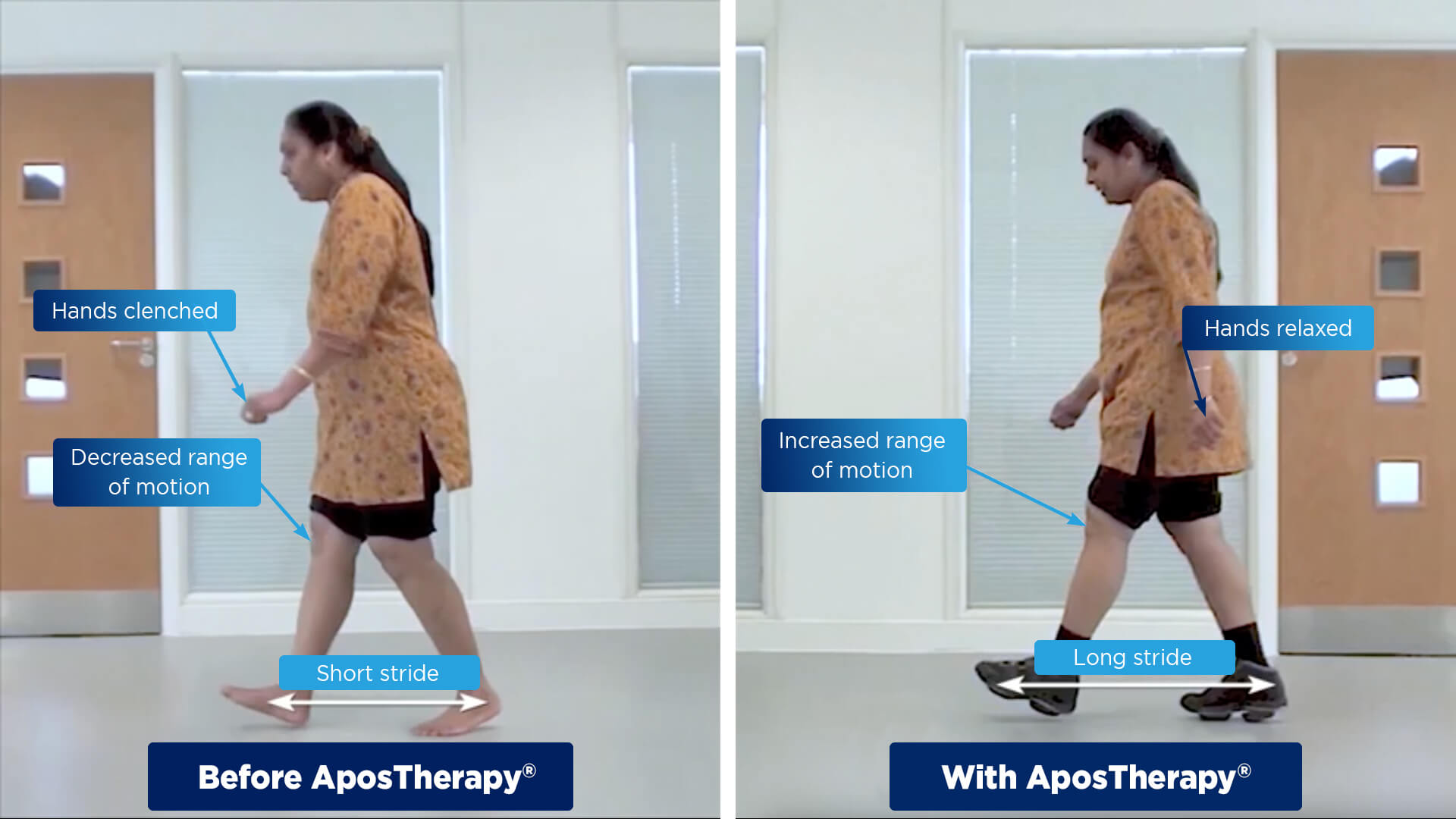
Before and After AposHealth®
In the video below you witness as patients with knee osteoarthritis go from struggling to get across the room to walking with confidence. Before and

Rheumatoid Arthritis vs Arthrosis (Osteoarthritis): What’s the Difference?
When talking about rheumatoid arthritis and arthrosis – which is more commonly called osteoarthritis – it can be confusing to someone who does not understand

Knee Pain Going Down Stairs? Here’s What You Need To Know
One of the most frequent complaints about knee pain is of aching when climbing up and down stairs. So, while taking the stairs is undoubtedly

AposHealth® Helps UK Head Soccer Coach Succeed
Natasha Orchard-Smith has a pretty unusual job; she’s the head coach of Arlesey Town, a semi-pro men’s soccer club in the UK. As of 2018,
Can Arthritis Be Cured? Not Yet, but That’s Not the Whole Story
Often when people ask whether there is a cure for arthritis, what they really want to know is whether there is a way for people

Introduction to Water Therapy & Aquatic Therapy for Adults With Joint Pain
You might know aquatic therapy by one of its other names, such as water therapy, pool therapy, or hydrotherapy. For people who suffer from joint

Random Knee Pain Isn’t Random: 6 Common Causes
Knee pain is a common issue that affects many of us at some point in our life. In some cases, the causes are pretty obvious
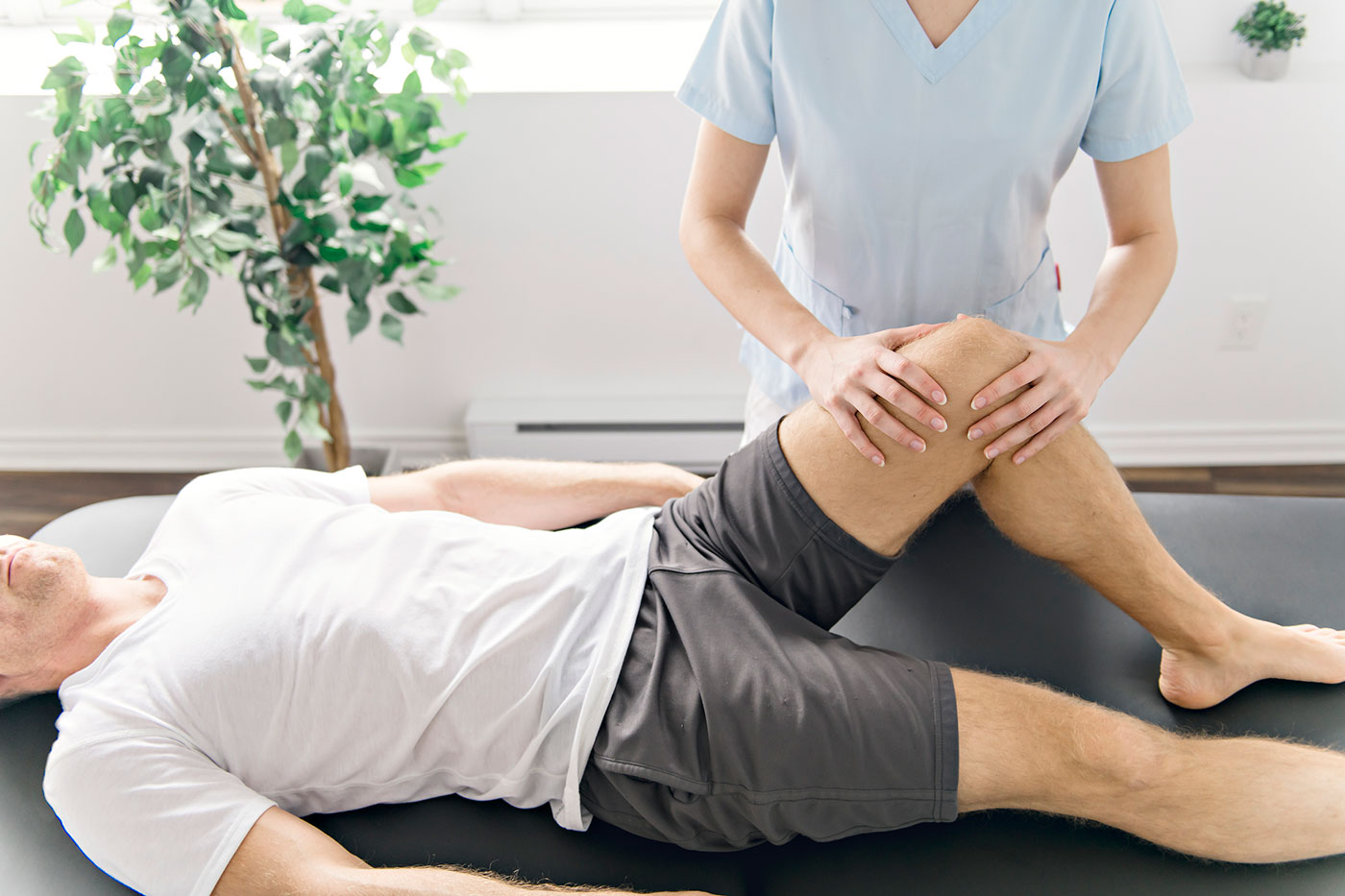
What Clinical Research Says About New Joint Pain Treatments
New joint pain treatments are ever-improving to help alleviate chronic pain and increase mobility. With current medical guidelines recommending a variety of options including physical

Knee Strengthening Exercises for Osteoarthritis
When everyday activities make your arthritic knee feel stiff and sore, exercising your knee may seem like the last thing you’d want to do. However,

Hyaluronic Acid Injections: Do They Work for Knee Arthritis?
Getting hyaluronic acid injections in the knee is a popular way to ease knee pain. By employing one of the body’s naturally-occurring lubricants, hyaluronan, hyaluronic

Addressing Knee Pain Head On – 4 Ways to Actively Reprogram Your Body
There is nothing wrong with you for experiencing knee and/or lower back pain, but there might be something wrong with the way your body and

Knee Osteoarthritis – The Most Common Culprit of Knee Pain
Knee Osteoarthritis, or knee OA, is one of the most common types of arthritis and a main cause of disability among adults, and it’s on
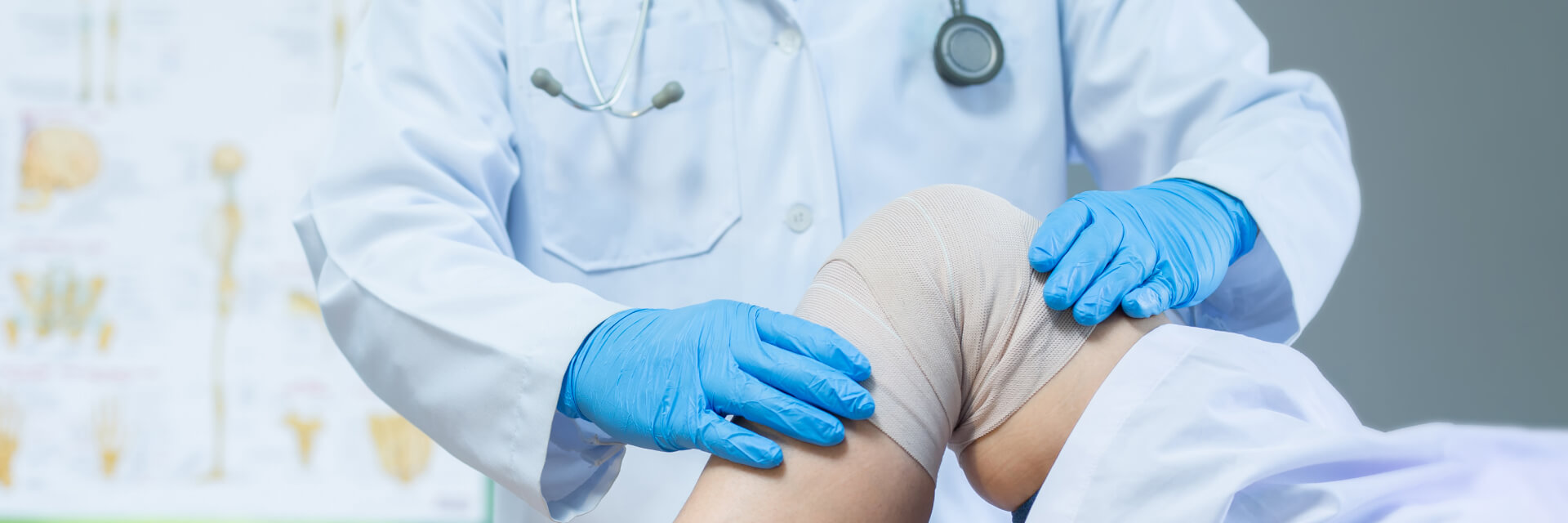
12 Hidden Costs of Delaying Knee Osteoarthritis Treatment
Still ignoring knee pain? You may be risking these 12 hidden costs of delaying treatment for knee osteoarthritis.

[Watch] Effortless Success – How AposHealth® Works Without You Changing Your Routine
People have been wondering how AposHealth® improves walking patterns (gait) while patients go about their regular routines. This is how the AposHealth footworn device re-educates

Wellness in the Workplace Means Planning Out Your Work Space
Sitting for long stints at the office can have painful effects. Here are some ways to avoid the dreaded burden of chronic lower back pain while at work.

How Gait Analysis Can Help Relieve Knee Pain
Whether your goal is to treat painful knee osteoarthritis or to gain an edge in the hundred-yard dash in the next Olympic Games, a thorough

Little-Known Tips to Cope with Knee Pain During Day-To-Day Activities
Using the stairs, standing up from a sitting position and walking around shouldn’t be so painful. Here are some little-known tips to help you cope better.
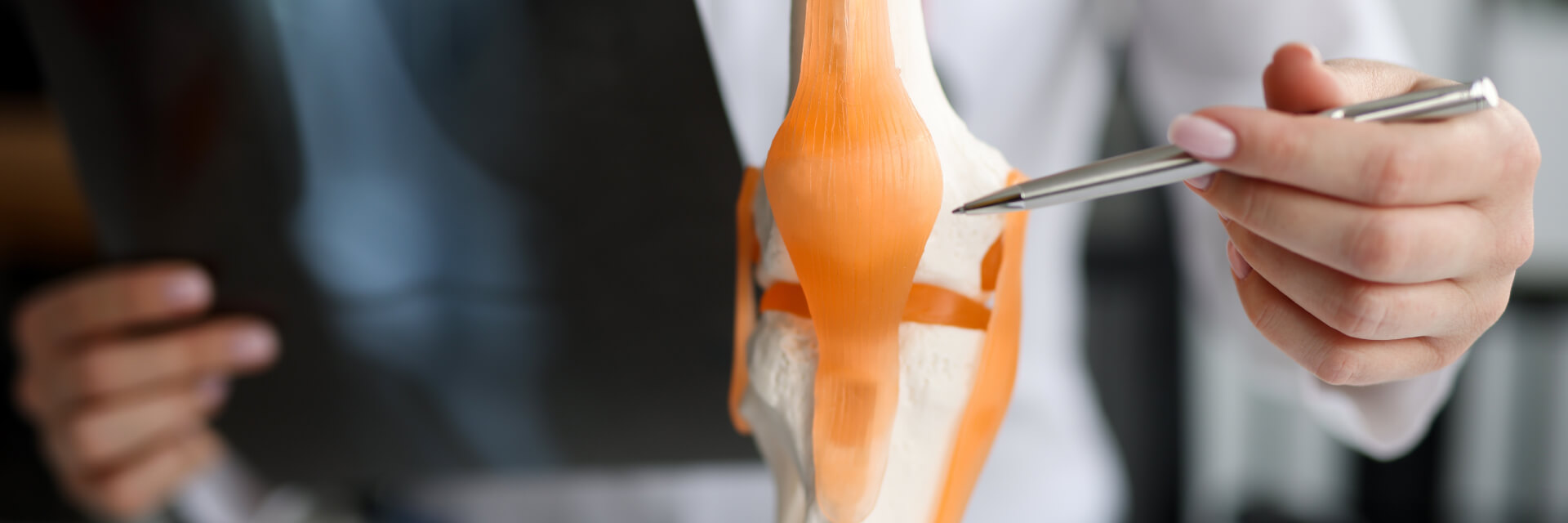
This One Principle Makes Joint Pain Much Easier to Understand
Why do some joints become painful and dysfunctional, while others remain healthy? Scientific evidence suggests the role of biomechanics may be more significant than once thought.

Can Losing Weight Prevent Knee Pain?
While obesity can put you at a higher risk of knee joint deterioration, can losing weight help decrease the rate of deterioration? And how much weight must one lose?

