We’ve all experienced physical pain in some capacity or another. At the moment that we’re injured, and for some time after, the pain can be sharp and completely overpowering. Even a relatively small injury can make it difficult for many of us to focus on mundane daily tasks.
And although many injuries heal naturally and return to typical function, not all do.
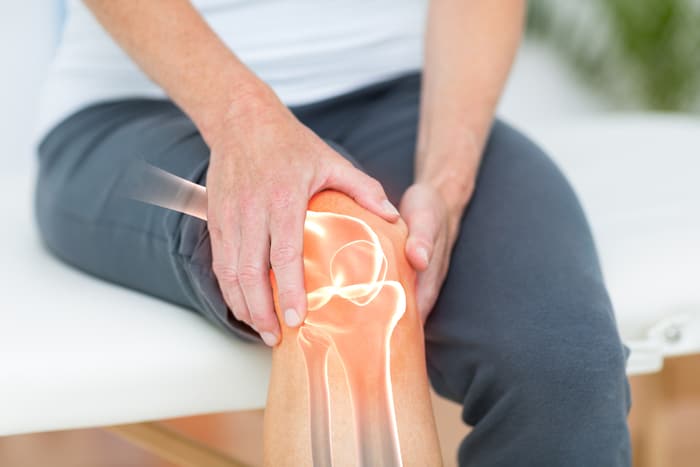
What Causes Chronic Knee Pain?
The weight-bearing joints of the lower extremities (i.e., the lower back, hips, and knees) are the most susceptible to developing arthritis, especially with advancing age. Wear and tear on the knee joint is a natural course of the aging process, but in some instances the wear and tear process occurs more quickly. That is osteoarthritis, one of the most common diagnoses of knee pain. This may occur due to excessive force on certain parts of the joint, muscle weakness, injury, faulty activity patterns or sudden increases in force on the joints.
Your knee is the largest joint in your body and it’s the most likely to be affected by age-related changes. These affect the actual movement of the joint, provoking more changes to the muscle and bone alignment and throwing off your normal walking mechanics (gait). The more a weight-bearing joint is misaligned and misused, the faster the degenerative change. Over time it becomes painful to carry out any weight-bearing activity, leading people to become less mobile so as to avoid experiencing pain.
However, lack of activity causes further deterioration and muscle weakness, increasing the disability of the joint which is what began all these problems. This is what the industry commonly refers to as the ‘pain cycle’.
10 Ways to Treat Chronic Knee Pain
We’ve simplified the various treatment options for people suffering from chronic knee pain into five broad approaches to chronic pain management.
Treatment for chronic knee pain can be grossly categorized as invasive and non-invasive. The most invasive treatment is total knee replacement surgery, or TKR.
Most of the suggestions listed here are non-invasive, including AposHealth®, injections, physical therapy, and weight loss.
NSAIDs (such as Aspirin / Ibuprofen)
NSAIDs, or non-steroidal anti-inflammatory drugs, are used to treat fever, inflammation, and general pain. They are available over the counter, are generally not expensive and can provide temporary relief. NSAIDs can also help bring down swelling and inflammation in the knee joints to ease knee pain, however, they don’t address the biomechanical cause of the pain.
Side effects may include but are not limited to: heartburn, stomach ulcers, high blood pressure, leg swelling, headaches, and dizziness, ringing in the ears, allergic reactions, and liver problems.
R.I.C.E
R.I.C.E. is a useful acronym to remember how to treat an injured or painful joint to decrease inflammation and pain and reduce the need for drugs. It stands for Rest, Ice, Compression, and Elevation, and it’s an easy way to deal with knee injuries or knee pain attacks anywhere, without special equipment or medication, but it does provide only short-term symptom relief without affecting the source of the pain and needs to be reapplied frequently. Ask your health care provider how to use R.I.C.E. safely and effectively.
Lifestyle Management
Here are four lifestyle changes that can improve one’s quality of life and relieve knee pain, although they don’t address the biomechanical roots of the pain. These changes are affordable and mostly don’t require the help of a specialist, but you’ll need to stick to it for them to have an effect, and they aren’t generally sufficient for moderate or severe pain:
- Stop smoking. Although smoking does not directly damage bones and joints, it constricts your blood vessels to bones, muscles and joints and slows down their healing processes, reduces their ability to absorb calcium and slows their production of bone-forming cells. It also damages airways, harming the circulation and respiratory systems that help the body heal.
- Get mobile. Increasing physical activity can have positive effects on the entire body, boosting overall health. Contrary to popular belief, the right movements can ease pain by maintaining bone and muscle health, not make it worse. If you have been avoiding certain movements and activities for a while, talk to a physical therapist and learn about safe ways to get moving.
- Reduce stress. Untreated stress, continual anxiety, and high worry levels can lead to heart problems, diabetes, and even obesity, all of which can make knee pain worse.
- Improve sleep. Sleep is your vital “off” time that your body needs to heal itself. The Centers for Disease Control and Prevention (CDC) recommends getting 7-9 hours of sleep per night for the average adult.
Diet Modification

Diet modification is another type of lifestyle choice that improves your quality of life but it deserves a mention on its own. Diet modification can help with weight loss which has been proven to improve knee pain and decrease the amount of knee joint deterioration, and can even save money on unhealthy processed foods. There are claims that diet modification can also help decrease inflammation of painful joints, and there are a wide variety of diet plans and support groups. However, it can be time-consuming to cook healthy, and you may need to allow time for your mind to change its definition of “tasty” food.
Alternative Medicine

Alternative medicine includes acupuncture, massage, meditation, and using vitamin and herbal supplements, which are often less painful and invasive than other treatments. Not all of these practices are built on science and they may not be covered by insurance, so check with your physician before making any dramatic changes based on alternative medicines.
Physical Therapy
Physical therapy includes a variety of approaches meant to be used in tandem to target dysfunction. Physical therapy is a patient-centered approach using evidence-based treatment with a focus on movement and function rather than medication. It should always be carried out by a licensed physical therapist, and some are better than others so it’s important to do your research first, and check your insurance because some policies have a yearly therapy cap. Bear in mind that you’ll need to learn the exercises and stick to them. Physical therapy can include:
- Soft tissue massage, i.e. localized massage and muscle work to temporarily relax the muscles.
- Stretching of the muscles to enable optimal tension and force generation during muscle contraction and stretch tight or restricted connective tissue.
- Thermal, electronic, or mechanical energy treatments like TENS, ultrasound, hot/cold compresses, and cold laser therapy. They’re clinically proven to be most effective when used in tandem with soft tissue work, stretching, and regular therapeutic exercise.
- Therex, or “therapeutic exercise,” is when a therapist creates a personalized, logical treatment plan of progressively difficult exercises to target specific areas of weakness and dysfunction. Compliance with the prescribed exercises at home has the most benefit in the long-term and is often the most difficult for patients.
Prescription Medication
Prescription medication, notably opioids, offer pain relief for joint pain, which often allows patients to increase their mobility without pain. However, prescription painkillers don’t directly improve joint function, do not address the root cause of the pain and the pain relief can be short-lived. Although opioids are effective for pain relief, they can have side effects, particularly the risk of addiction as the body adjusts to the medication and requires progressively higher doses to keep pain at bay.
Joint injections
Corticosteroids or hyaluronic acid options, such as Supartz, can be injected directly into the knee joint, relieving pain and inflammation to help restore mobility. Although pain relief is usually immediate, the effects wear off with time. There’s also a limit to the number of injections one can safely receive within a particular time period, and it doesn’t address the biomechanical issues.
Surgery
Common types of knee surgery include arthroscopic surgery, partial knee resurfacing and total knee replacement surgery (TKR). Not everyone is eligible for knee surgery, depending on their level of disability and underlying health conditions. Surgery alone will not magically solve chronic knee problems. It needs to be followed by professional rehabilitation. You will also still need to follow many of the lifestyle changes mentioned above, retrain the muscles to properly support the body and the new joint to maintain your function. If you have TKR at a young age, you might need a repeat operation decades later when your replaced joint “wears out.”
Three types of knee surgery include:
- Arthroscopic surgery is the least invasive type of joint surgery, so it’s also the fastest and the one that needs the shortest amount of recovery time. It involves inserting a small camera and mini surgical instruments into the joint to diagnose and treat joint problems. It’s commonly used for removal of loose fragments of tissue, or the removal of a torn meniscus or repair of a recently torn ACL.
- Partial knee resurfacing is less invasive than a full knee replacement and usually recommended for people with limited joint damage. It involves replacing only the diseased surfaces of the joint with artificial implants, instead of the entire joint, so it has a shorter recovery time than TKR.
- Total knee replacement or TKR is the most invasive form of knee pain treatment. During the surgery, a completely artificial joint replaces the existing dysfunctional joint. Like all surgery, it carries a number of health risks and not everyone is eligible for it, so it’s usually a last resort. The surgery itself typically takes 1-2 hours, but it can take over a year before you start to feel the benefits.
AposHealth®
AposHealth® is an innovative, research-based therapeutic walking program that is clinically proven to improve muscular control and coordination, relieve knee pain, and improve knee and muscle function through personalized biomechanical shoes. It’s non-invasive, safe41, evidence based, and easy to do at home alongside your daily tasks. You’ll receive a thorough gait assessment by an AposHealth® trained clinician, and if you are accepted into the program, you will receive your own customized footworn device. AposHealth® is currently only available in specific locations and is covered by some insurance plans.
Choosing a Knee Pain Treatment That Fits
As you can see, there are a lot of ways that you could try to treat knee pain, but also may carry various risks and lifestyle changes. Each person’s body is different and each person’s response to treatment is different, too, so what works for one person might not work for the next one. What matters is that you ask your care provider questions about each method, and do your research to find the treatment that works best for you.
AposHealth® uses a personalized footworn device to redistribute the pressure away from the painful area of your joints, improve your movement patterns and build your muscles’ control and coordination. The footworn device is designed to re-educate your muscles to move with improved mechanics. Over time, your body gains better muscle control and coordination and learns to maintain the improved movement patterns even when you’re not wearing the device.
The AposHealth® foot-worn device is FDA-cleared for treating knee osteoarthritis, to help temporarily reduce knee pain and improve lower extremity function during activities of daily living. It is also a non-FDA cleared wellness device which can help patients live well with other musculoskeletal conditions such as chronic low back and hip pain.


